Our latest articles
Costochondritis Rehabilitation and Prevention
Inflammatory costochondritis is in most cases caused by a lack of fitness, hunched posture, spinal stiffness or hypermobility, fear of movement and activity aggravating pain and ergonomically disastrous workstations and unhealthy lifestyle choices.
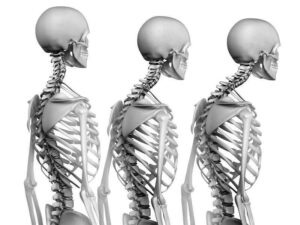
The best way to treat or prevent it is to choose and implement healthy ergonomics (sit/stand desks), get professional help from an experienced osteopath, chiropractor or physiotherapist to reset your posture, move frequently, start a good diet (tending to vegetarianism) and graduated, regular non-impact exercise until you recover fully.
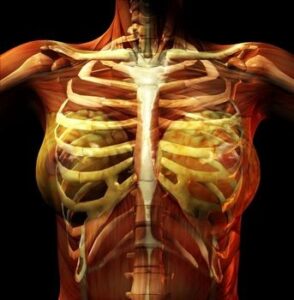
 When you’re sitting at work or at home scoop your chest in and push it out – then make circling movements with your chest, first one way and then the other. Do breaststroke and backstroke movements every half an hour for a few seconds to mobilise your shoulders, ribs and chest and maintain movement and flexibility and to remind you to sit upright. Set your screen at eye-level to stop you dropping your chest or poking your chin forwards.
When you’re sitting at work or at home scoop your chest in and push it out – then make circling movements with your chest, first one way and then the other. Do breaststroke and backstroke movements every half an hour for a few seconds to mobilise your shoulders, ribs and chest and maintain movement and flexibility and to remind you to sit upright. Set your screen at eye-level to stop you dropping your chest or poking your chin forwards.
Source : NHS
Surgery for Costochondritis
Proper rehabilitation of posture, mobility, fitness and exercise is the best option before any medical drug or cortisone injection intervention is even considered and certainly before surgical removal of the sore cartilage as absolutely the last resort.
Ideally start a course with a combination of expert physical therapy, chiropractic or osteopathic joint manipulation, connective-tissue mobilisation and postural rehabilitation for your costochondritis.
Source : NHS
Medications for Costochondritis
Costochondritis inflammation may respond to some extent to nonsteroidal anti-inflammatory medications (NSAIDS) such as ibuprofen (Advil or Motrin) and naproxen (Aleve) but they should never be used long-term as these medications have potentially serious side-effects. You may be offered a local anesthetic and steroid injection in the area that is tender if normal activities become extremely painful and the pain does not respond to drugs but any effect will be short-lived .
There is absolutely no place for long-term use of anti-inflammatories, muscle relaxants, powerful codeine / morphine based opioid addictive painkillers or gabapentin, pregabalin or amitriptyline along with a host of antidepressants commonly prescribed in low-doses as ‘pain-relief’ which just cover-up symptoms and perpetuate musculoskeletal problems into very long-term, unresolved pain, ill-health, inactivity, obesity and misery.
Infectious (bacterial or fungal) costochondritis should be treated initially with intravenous (in the vein or IV) antibiotics. Afterward, antibiotics by mouth or by IV should be continued for another two to three weeks to complete the therapy.
In most cases, manual treatments, if applied by an expert, will improve joint, muscle and musculoskeletal connective-tissue fascial function which relieves pain. Full postural rehabilitation with regular specific exercises and longterm improved fitness will aid a long-term cure.
Source: NHS
Home Remedies for Costochondritis
The following home remedies may provide some relief from costochondritis:
Taking pain relievers such as nonsteroidal anti-inflammatory medications like ibuprofen (Advil, Motrin) or naproxen (Aleve) as needed.
Using local heat or ice to relieve pain.
Avoiding unnecessary exercise or activities that make the symptoms worse; avoiding contact sports until there is improvement in symptoms, and then returning to normal activities only gradually and as tolerated.
Doing stretching exercises.
Source: NHS
Exams and Tests for Costochondritis
There is no specific test for diagnosing costochondritis. The patient’s medical history and a physical exam are the mainstays of diagnosis. So, if the onset of your chest pain or costochondritis was following a traumatic event, an impact or lifting heavy weights in the gym, someone barging into you or after weeks of intense study for exams sitting with poor posture in bed or scrunched up on the sofa, then the likelihood is it’s mechanical or postural and you don’t need the intense barrage of extremely expensive, time consuming and worrying tests and investigations which are commonly done, regardless of the logical and extremely likely physical nature of the diagnosis.
The doctor will press on your chest to reproduce tenderness over the affected rib joints, usually over the fourth to sixth ribs in costochondritis, and over the second to third ribs in Tietze syndrome. In costochondritis with unknown causes, there is no apparent swelling of the costochondral joints, although there is swelling and tenderness of the rib-cartilage junctions in Tietze syndrome. Some doctors use the terms costochondritis and Tietze syndrome interchangeably but Tietze syndrome has a sudden onset without any preceding respiratory illness or any history of minor trauma and there is frequently radiation of pain to arms and shoulders, as well as pain and tenderness associated with swelling at the point that hurts.
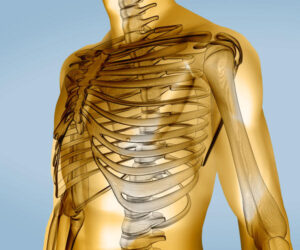
Tests are sometimes needed to rule out other conditions that have similar symptoms but are more worrying, like heart disease. So if you’re overweight, inactive and diabetic, your blood pressure is high, your diet is designed to make you ill and you take a lot of medication, then heart disease is a clear possibility and needs to be investigated.
Blood tests and a standard chest X-ray are usually not helpful in diagnosing costochondritis.
However, after sternum surgery, or for people at risk for heart disease, doctors will be more likely to do tests if you have chest pain and possible costochondritis to be certain you do not have any infection or other serious medical problems.
To determine if infection is the cause of chest pain, doctors will:
Look for signs of infection such as redness, swelling, pus, and drainage at the site of surgery
Order a more sophisticated imaging study of the chest called a gallium scan, which will show increased uptake of the radioactive material gallium in an area of infection
Check the white blood cell count to see if it is elevated, a sign of infection
Order a chest X-ray if pneumonia is a suspected cause of chest pain
Order an ECG and other tests if a heart problem is suspected
Costochondritis is a less common cause of chest pain in adults but occurs fairly frequently in people who have had chest drains or cardiac surgery. The diagnosis can only be reached after excluding more serious causes of chest pain that are related to the heart and lungs. The appropriate studies, such as ECG, chest X-rays, blood test for heart damage, and other studies will be done as indicated. Any chest pain in adults is taken seriously and not ignored. If you are concerned, consult your doctor.
Source : NHS
When to Seek Medical Care
Call the doctor for any of the following symptoms:
– Trouble breathing
– High fever
– Signs of infection such as redness, pus, and increased swelling at the rib joints
– Continuing or worsening pain despite medication
– Nausea
– Sweating
Go to a hospital’s emergency room if you have difficulty breathing or any of the following symptoms occur.
These symptoms are generally not associated with costochondritis:
– High fever not responding to fever-reducers such as acetaminophen (Tylenol) or ibuprofen (Advil)
– Signs of infection at the tender spot, such as pus, redness, increased pain, and swelling
– Persistent chest pain of any type associated with nausea, sweating, left arm pain, or any generalized chest pain that is not well localized. These may be signs of a heart attack. If you are not sure what is causing your condition, always go to the emergency room.
Source: NHS
Costochondritis Causes
- Costochondritis is an inflammatory process which is commonly caused by musculoskeletal dysfunction of the rib joints at the back where they attach to the thoracic spine and at the front in the chest where they attach to cartilage. This is universally due to long-term poor posture with a stiffening, rounded, kyphotic middle-back from slumping in sofas or dropping the chest and poking the chin forward and sitting at computer screens that are too low and texting on mobile phones.
- Repeated minor trauma to the chest wall, overuse of the arms, or viral respiratory infections can commonly cause chest pain due to costochondritis. Occasionally, costochondritis as a result of bacterial infections can occur in people who use IV drugs or who have had surgery to their upper chest. After surgery, the cartilage can become more prone to infection, because of reduced blood flow in the region that has been operated on.
Different types of infectious diseases can cause costochondritis.
Viral: Costochondritis commonly occurs with viral respiratory infections because of the inflammation of the area from the viral infection itself, or from straining from coughing.
Bacterial: Costochondritis may occur after surgery and be caused by bacterial infections.
Fungal: Fungal infections are rare causes of costochondritis.
Source : NHS
Costochondritis Symptoms
Chest pain associated with costochondritis is usually preceded by exercise, minor trauma, or an upper respiratory infection.
The pain, which may be dull, usually will be sharp and located on your front chest wall. It may radiate to your back or abdomen and is more common on your left side.
There can be pain with a deep breath or cough.
The most common sites of pain are your fourth, fifth, and sixth ribs. This pain increases as you move your trunk or take deep breaths. Conversely, it decreases as your movement stops or with quiet breathing.
The reproducible tenderness you feel when you press on the rib joints (costochondral junctions) is a constant feature of costochondritis. Without this tenderness, a diagnosis of costochondritis is unlikely.
Tietze syndrome, on the other hand, exhibits swellings at the rib-cartilage junction. Costochondritis has no noticeable swelling. Neither condition involves pus or abscess formation.
Tietze syndrome usually affects the junctions at the second and third ribs. The swelling may last for several months. The syndrome can develop as a complication of surgery on your sternum months to years after the operation.
When costochondritis occurs as a result of infection after surgery, you will see redness, swelling, or pus discharge at the site of the surgery.
Source : NHS